Stroke in the US
Every 40 seconds, someone in the US suffers a stroke1*

Every year in the US, there are an estimated 795,000 strokes and an estimated 163,000 deaths are due to strokes1*
Stroke is the fifth leading cause of death in the US and a major contributor to long-term disability and dementia.1 Stroke leaves an emotional imprint on survivors, their families, and care partners.2-5
*Incidence is based on Greater Cincinnati/Northern Kentucky Stroke Study and National Institutes of Neurological Disorders and Stroke data for 1999 that was compiled by the National Heart, Lung, and Blood Institute (NHLBI). Mortality is based on NHLBI tabulation using the National Vital Statistics System.
The burden of ischemic stroke
Most strokes are caused by clots that do not originate in the heart6
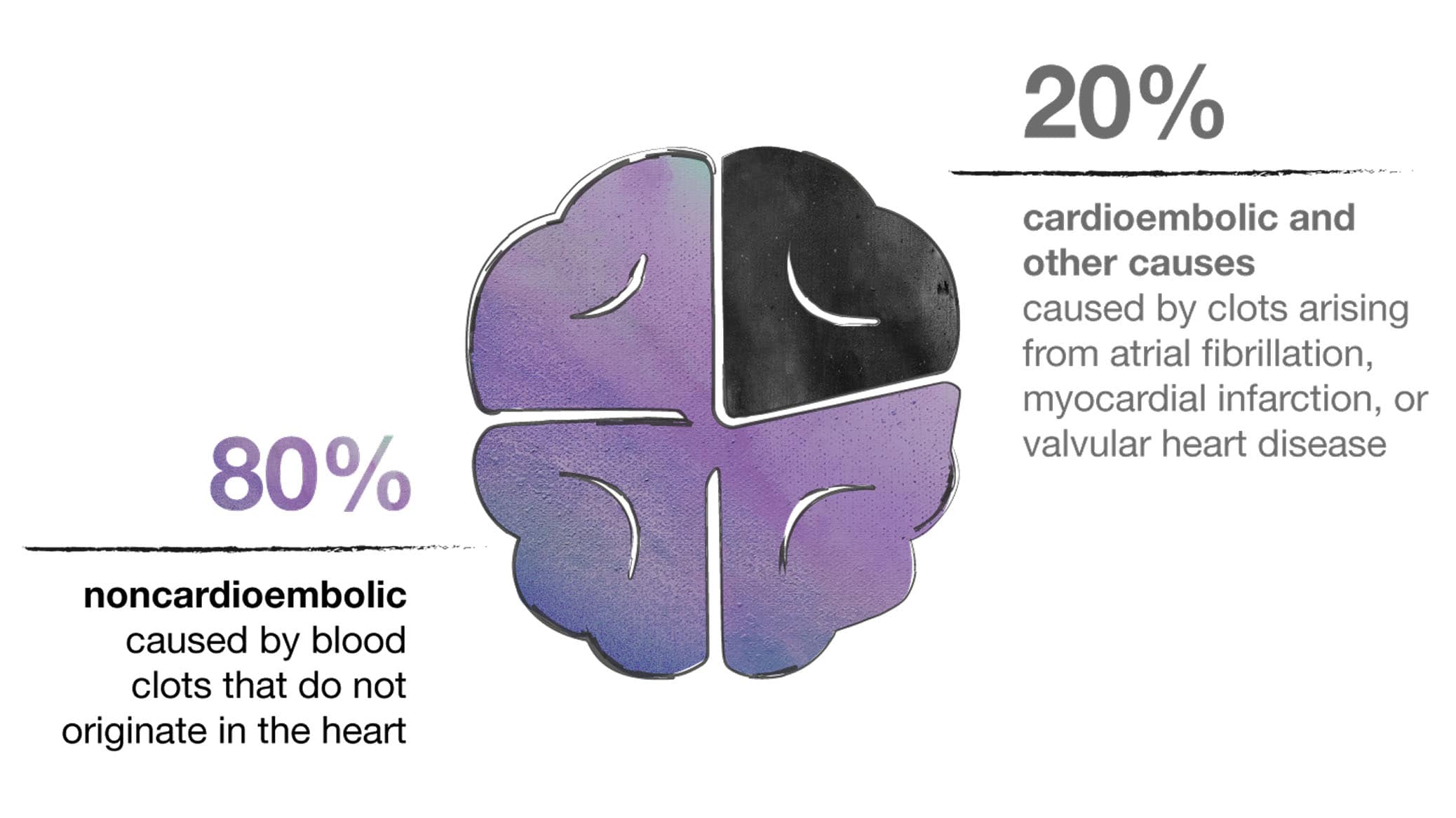
Acute ischemic strokes and transient ischemic attacks (TIA) occur when blood flow to part of the brain is reduced or blocked, typically due to a thromboembolism traveling to the brain or stenosis of a cerebral artery.7-9 This causes significant, often irreversible brain tissue damage—leading to short- and long-term mental and physical consequences that make stroke so damaging.7

Recurrent strokes are common
Approximately 1 in 5 ischemic stroke survivors will have another stroke within 5 years, and ~1 in 10 will have another stroke within 1 year, despite secondary stroke options.10-12
Recurrent and more severe ischemic strokes tend to be more disabling, and increase the risk of dementia.13,14
Survivors with higher disability scores after an ischemic stroke are also more likely to suffer subsequent strokes and major cardiovascular events.15-17
Recurrence of ischemic stroke significantly increases the risk of death18
While secondary prevention strategies have improved recurrence rates, death from recurrent stroke remains high.18
Age, race, and socioeconomic factors affect the rates of stroke recurrence19-21
The risk of secondary stroke increases in marginalized groups, who may suffer disproportionately from healthcare inequity. Older people, Black adults, and those of low socioeconomic status all have an increased risk of suffering a second stroke.19-21
According to an observational study (N=3816) in Cincinnati, Ohio, socioeconomic and health inequities likely contributed to higher prevalence of risk factors.21

Secondary stroke deserves another look
Approximately 1 in 5 ischemic stroke survivors will have another stroke within 5 years, despite available secondary stroke prevention options.10,11
- Martin SS, et al. Circulation. 2024;149(8):e347–e913.
- Liu L, et al. PLoS Med. 2023;20(3):e1004200.
- Rafsten L, et al. J Rehabil Med. 2018;50:769–778.
- Janssen EPJ, et al. J Psychosom Res. 2024;187:111914.
- Broomfield NM, et al. J Neurol Neurosurg Psychiatry. 2022;93:886-894.
- Schneck MJ. Cardioembolic stroke. June 7, 2021. Accessed November 16, 2021. https://emedicine.medscape.com/article/1160370-overview
- Kuriakose D, Xiao Z. Int J Mol Sci. 2020;21:7609.
- Bir S, Kelley RE. Biomedicines. 2021;9:1906.
- Guzmán JD. Neurologia. 2012;27(Suppl 1):4–9.
- Kolmos M, et al. J Stroke Cerebrovasc Dis. 2021;30(8):105935.
- Lakshminarayan K, et al. Stroke. 2011;42(6):1556–1562.
- Wang Y, et al. PLoS ONE. 2023;18(8):e0289790.
- Koton S, et al. JAMA Neurol. 2022;79(3):271–280.
- Hobenau C, et al. Lancet Neurol. 2022;21(10):889–898.
- Havenon A, et al. JAMA Netw Open. 2024;7(7):e2423677.
- Du J, et al. J Am Heart Assoc. 2024;13(3):e030702.
- Park JH, et al. Eur J Neurol. 2016;23(2):361–367.
- Chen C, et al. Ann Neurol. 2024;96:332–342.
- Albright KC, et al. Neurology. 2018;91(19):e1741–e1750.
- Becker CJ, et al. Neurology. 2024;102(11):e209423.
- Robinson DJ, et al. Neurology. 2022;99(22):e2464–e2473.



